Osteoarthritis Surgery and Joint Replacement
The most common type of arthritis is osteoarthritis. It causes symptoms like pain, swelling, stiffness, and decreased flexibility in joints. You can develop osteoarthritis as a result of joint injury, overuse, increasing age, and other factors. Since osteoarthritis can’t be reversed, preventing it is key.
For those living with osteoarthritis joint damage, finding a treatment that improves mobility and quality of life is important. Osteoarthritis self-care treatments and exercises can be used in the condition’s early stages to help relieve your pain and slow the disease’s progression.
Some people will need osteoarthritis surgery or total joint replacement for osteoarthritis to live their best life.
Osteoarthritis Symptoms
The soft, rubbery substance that covers the ends of bones is called articular cartilage. Osteoarthritis causes it to wear away, which leads to the bones of that joint rubbing together during movement.
According to the Centers for Disease Control (CDC), osteoarthritis affects approximately 1 in 5 US adults. This degenerative joint disease typically comes on slowly and gets worse with time.
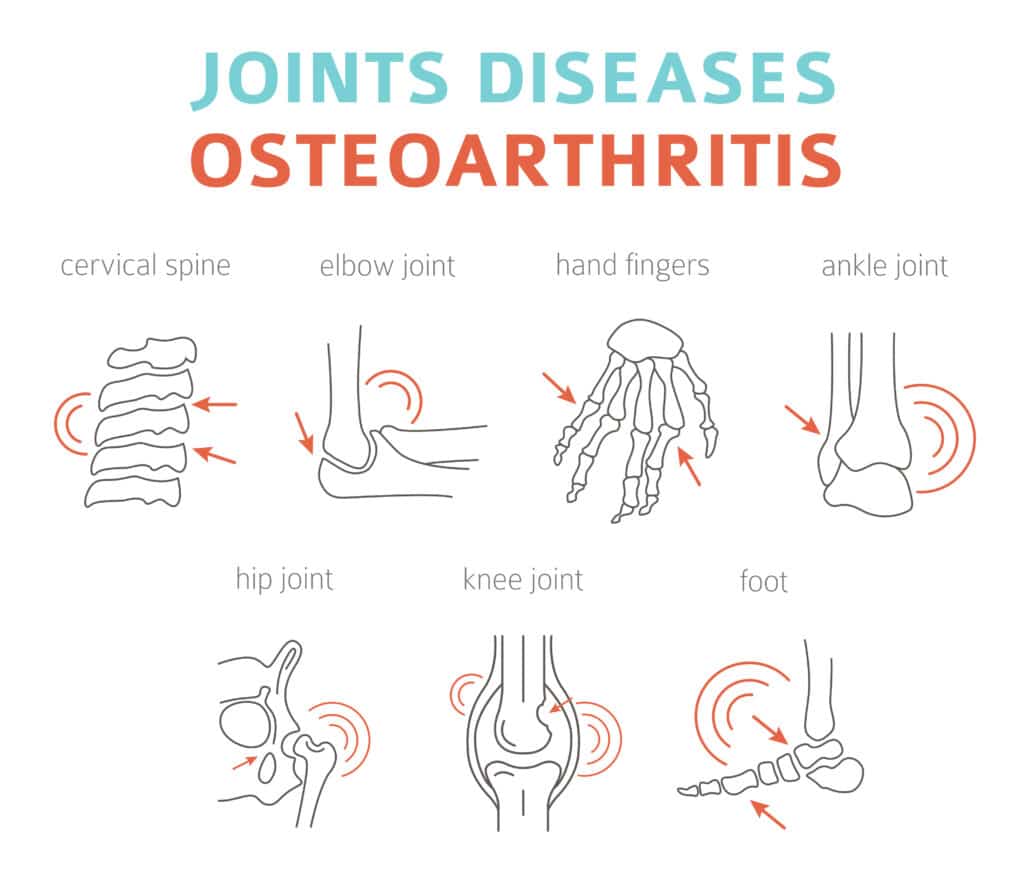
Joints with osteoarthritis (OA) can get so stiff that daily tasks become difficult, and the pain and disruption can negatively impact mental health.
The joints that develop OA most often include the following:
- Hands and feet, particularly the ends of the fingers and toes and the base and ends of the thumbs and big toes
- Knees
- Hips
- Back and neck, particularly the cervical spine
- Elbows
- Ankles
Osteoarthritis self-care techniques like physical therapy, supplements, and medications, alongside lifestyle changes such as exercise and losing weight, can be helpful tools for managing osteoarthritis.
For some living with severe osteoarthritis, surgery may become a necessary option for improving quality of life. Osteoarthritis knee surgery, osteoarthritis hip surgery, osteoarthritis shoulder surgery, and osteoarthritis thumb surgery are the most common types of OA surgery.

5 Types of Osteoarthritis Surgery
Work with your orthopedic knee, hip, and shoulder surgeon to determine which of the many types of osteoarthritis surgeries is right for you. Together, you will find the right procedure based on your symptoms and desired outcomes.
1. Arthroscopy
Arthroscopy for osteoarthritis is a surgery that begins with your orthopedic surgeon inserting a small camera on a flexible tube into your joint. Aided by the camera, your surgeon can smooth rough spots, remove cysts or bone fragments, and get rid of damaged cartilage.
Arthroscopic surgery for osteoarthritis is relatively quick in both procedure and recovery time. The best candidates for osteoarthritis arthroscopy are typically active individuals under 40. Arthroscopy may be a better fit for soft-tissue injuries rather than arthritic issues.
2. Total Joint Replacement Osteoarthritis Surgery
Those undergoing total joint replacement for osteoarthritis, also called arthroplasty, can expect to have their damaged joint removed and replaced with an artificial joint made of plastic, ceramic, or metal. Total shoulder joint replacement, total hip joint replacement, and total knee replacement surgery are most common.
To many, the idea of undergoing total joint replacement (TJR) can be intimidating. However, total joint replacement has come a long way in recent years.
Many people undergoing TJR will undergo the procedure as outpatients, not even needing to stay overnight in the hospital. Surgeons can also sometimes use minimally invasive techniques, leading to less pain and shorter recovery time. These techniques also require less cutting of surrounding tendons and joints, improving pain and joint replacement recovery expectations.
In addition to surgical procedures, there have been improvements in analgesia and anesthesia. A mix of medications that help with reducing pain and swelling alongside regional nerve blocks decreases the need for post-operative narcotics.

Improvements in imaging technology also help surgeons get a better view of the joint in real time. These advancements enable surgeons to make specific adjustments to the placement of the new joint that drastically improve joint replacement outcomes.
With all these advancements, many patients undergoing TJR are up and moving in a matter of hours. Movement and total joint replacement exercises help blood flow, which encourages healing.
It’s important to remember, however, that prosthetic joints can wear out over time, just like real ones. For this reason, many surgeons recommend delaying TJR when possible to avoid the need for repeat surgeries.
3. Joint Resurfacing
Joint resurfacing is a newer type of joint replacement surgery. In joint resurfacing, the damaged portion of the joint is removed and replaced. Knee resurfacing can relieve joint pain and improve function. Hip resurfacing is good for people who participate in high-impact sports or those requiring flexibility.
4. Osteotomy
An osteotomy involves cutting and removing bone near the damaged joint or adding a wedge of prosthetic bone to improve alignment or decrease pressure. This is a less commonly used surgery for osteoarthritis, but there may be certain conditions where it is the most appropriate.
5. Joint Fusion
In joint fusion surgery, your orthopedic surgeon will use pins, plates, screws, or rods to connect bones and make one solid joint. Over time, the joint’s bones will fuse, which eliminates range of motion and flexibility. Joint fusion surgery typically lasts forever, but it can increase stress on other joints and cause them to develop OA as a result.
If you have hip osteoarthritis, knee osteoarthritis, hand osteoarthritis, or any other type of OA and would like to speak with an orthopedic specialist about osteoarthritis surgery, please comment below or contact us.
Leave a Reply