Why Does My Knee Keep Popping Out of Place?
There are two types of patellar instability, which is, simply put, when the kneecap moves outside its normal space. One is traumatic patellar dislocation and the other is chronic patellar instability.
According to the Cleveland Clinic, some degree of patellar instability is relatively common in the US, estimated at 50 to 77 cases per 100,000 people.
Anatomy of the Knee
The kneecap (patella) is attached to the thigh bone (femur) and shin bone (tibia) by tendons. The patella fits into a notch (trochlear groove) in the femur. It moves up and down when you bend your knee.
Patellar instability is when the kneecap slips outside this groove and does not track the way it should. The patella may move entirely outside the trochlear groove (a dislocation) or only partly outside (a subluxation).
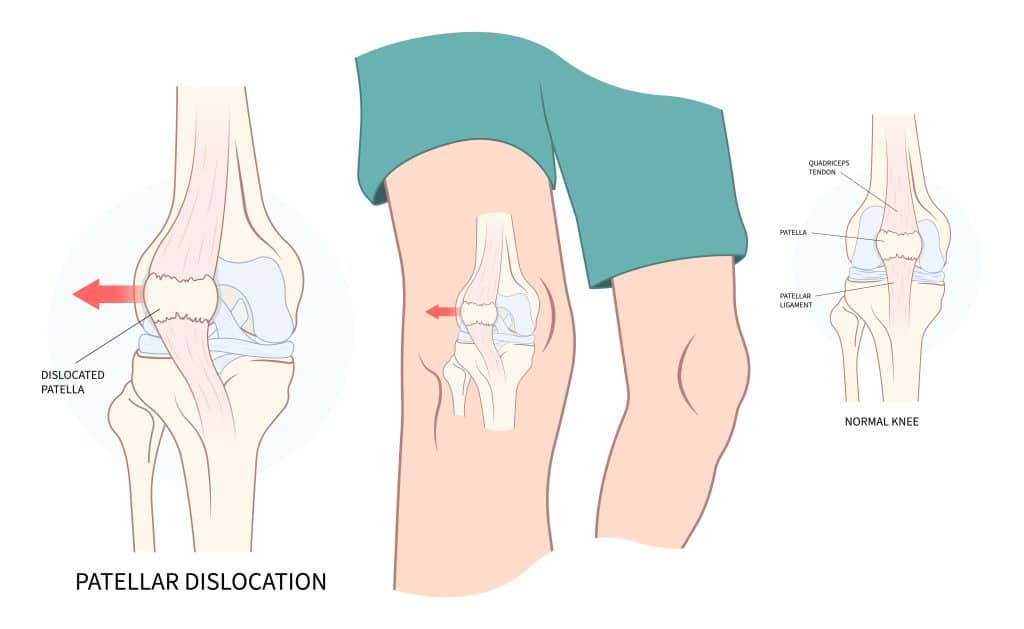
An injury, such as a fall playing sports or a sharp blow during a car accident, can cause patellar instability. It may also be caused by an anatomical issue, like a shallow or uneven trochlear groove that prevents the kneecap from aligning properly. Additionally, some people have loose ligaments that don’t hold the kneecap sufficiently during movement, which allows the joint to be overly flexible.
Patellar dislocation is often the result of an injury, although chronic patellar instability sometimes also leads to patellar dislocations over time.
Certain populations and people with various health conditions are more likely to develop patellar instability. These include:
- Women
- People in their teens and 20s
- Individuals with anatomical misalignments of the knee
- Overweight individuals
- Those with Cerebral palsy, Down’s syndrome, or Ehlers-Danlos syndrome
Patellar Instability Symptoms
A person with patellar instability may experience the following symptoms:
- Knee pain, stiffness, and swelling, similar to what is seen with osteoarthritis
- The sensation that the kneecap is not in its proper place
- Difficulty walking or the feeling that the knee cannot support one’s weight
- Buckling, catching, cracking, popping, or locking in the knee during movement
- A sensation of pain under the kneecap, especially during deep bends
- Obvious deformity of the knee
In some cases, the kneecap returns to its proper location on its own. In others, it must be manually moved back into place by a medical professional, such as an orthopedic knee specialist. This procedure is called a reduction, and you usually receive pain medication during this process to make it more comfortable.
Most cases are diagnosed through a physical exam and an X-ray. In some cases of traumatic injury, an MRI is used to evaluate whether surrounding structures have also been damaged.
How to Fix Patellar Instability
Many cases of patellar instability, including some patellar dislocations, are treated with straightforward non-surgical methods such as:
- Rest
- Ice (20 minutes per session, as needed)
- Elevation
- Nonsteroidal anti-inflammatory medicines (like aspirin or ibuprofen)
- Knee brace
- Crutches
- Physical therapy (to strengthen surrounding muscles)
Patellar Instability Surgery
If the kneecap does not stay in the proper location, is chronically unstable, or the dislocation is severe enough to damage surrounding cartilage, tendons, or ligaments, you may need surgery. In some instances, surgery is arthroscopic, whereas other cases require open surgery.
In arthroscopic surgery, your orthopedic knee surgeon makes small incisions and uses a tiny camera (arthroscope) and thin surgical instruments to complete the procedure.
If open surgery is the best option for your injury, you will work with your surgeon to choose the best surgery type. Some common surgeries for patellar instability include:
- Knee osteotomy to reposition the tibia and femur, thereby improving the knee’s movement and tracking
- Medial patellofemoral ligament (MPFL) repair to strengthen and repair the surrounding ligaments
- MPFL reconstruction, which replaces the damaged ligaments with a tendon from another part of your body or a donor
- Knee replacement to correct repeat dislocations
Full recovery from knee surgery can take 3 to 12 months, depending on the severity of your injury and the type of surgery used for treatment.
Prevention

Following non-surgical treatments, the recurrence rate of patellar instability ranges from 15 to 44 percent. The chance of additional dislocations increases to 50 percent if you’ve previously dislocated your knee.
Keep the muscles surrounding your kneecap strong to help prevent initial and repeated instances of patellar instability. Engage in regular, low-impact activities such as riding a bike or walking, and work with a sports medicine doctor to develop a routine of targeted patellar instability exercises. If you’re prone to an unstable knee, wearing a knee brace is a good idea. Over time, people with ongoing issues are more likely to suffer from chronic pain, limited range of motion, and arthritis, so prevention is key for long-term health and mobility.
If you have questions about knee pain or are concerned that your kneecap is unstable, please comment below or contact us. We are happy to answer your questions.
10 Comments
Permalink
Hello I’m 18 and my right knee is “bigger” than the other randomly. I think a bone is popping out more. I don’t do sports, or move that much so I didn’t get injured. I’m not overweight or underweight. It feels tense when I bend it, but there’s absolutely zero pain and I can walk, it just feels odd. I don’t know what it is.
Permalink
Ray, It’s great that you’re paying attention to your body. Even without pain, changes in size or tension can be worth getting checked out by a doctor. They can help determine the cause and suggest any necessary steps to keep your knee healthy.
Permalink
My knee usually cracks all the time
I feel pains when walking and also restlessness when I’m about to sleep
Sometimes while walking my knee moves out of place
I went to the doctor but he said my knee was fine
Please what else should I do?
Permalink
Hi Iara, it’s important to get a second opinion, especially if your symptoms persist or worsen. Cracking knees, pain when walking, and the sensation of your knee moving out of place could indicate underlying issues that need further evaluation. Consider visiting a specialist like an orthopedic surgeon or a physical therapist for a more detailed assessment. They may recommend imaging tests or physical therapy to help manage your symptoms.
Permalink
I’m 14 and about 3 months ago I got hit directly in the side of the knee with a softball and my knee hasn’t felt the same since. My one knee is bigger than the other and looks different it also pops lots and hurts on and off. Should I be concerned and got to the doctor about it?
Permalink
Hi Michelle, Yes, you should see a doctor, especially since your knee is still swollen, painful, and popping after three months. These symptoms could indicate something like ligament damage, cartilage injury, or another issue that needs medical attention. It’s best to get it checked out to prevent any long-term problems.
Permalink
My 12 year old daughter has had her kneecap pop out of place two times now. The Dr. said he doesn’t know if PT will help this last time and she will probably need surgery. There has to be another way to fix this problem. Do you know of any way to strengthen the knee and keep from needing surgery?
Permalink
Hi AJ, physical therapy can often be beneficial in strengthening the muscles around the knee, which might help stabilize the kneecap. Additionally, bracing and activity modification might reduce the risk of future dislocations. However, every case is unique, so it’s essential to discuss all available treatment options with a specialist to determine the best course of action for her specific situation. If you’d like, we can connect you with one of our orthopedic specialists for a second opinion.
Permalink
I was diagnosed of a spiking in my tibial spines. My left knee feels stiff and numbness sometimes runs through my feet and fingers of my left side. I have also been diagnosed of lumbar spinal stenosis and cervical spinal stenosis. I think I will really be fine if my the bone spurs in my left knee if treated. Physiotherapy has helped so much as far as my other diagnosis but the bone spurs has been a major problem for me especially with my mobility and balance. How can I really recover? I’m currently using a knee brace though
Permalink
Hi Rejoice, it’s essential to address both the bone spurs and underlying issues to improve your mobility and balance. We recommend consulting with an orthopedic knee specialist. In the meantime, continuing physiotherapy and using your knee brace can provide support. Feel free to contact us to schedule an appointment 435-615-8822.