Degenerative Disc Disease Self-Care
Though not considered a true disease, degenerative disc disease is a condition in which damaged spinal discs cause pain. The rubbery, shock-absorbing discs between each bone (vertebrae) in your spinal column act as cushions to help you stay flexible and allow you to move, bend, and twist without pain. Over time, nearly everyone’s spinal discs break down to some degree, but only those who develop symptoms from this natural process are considered to have degenerative disc disease.
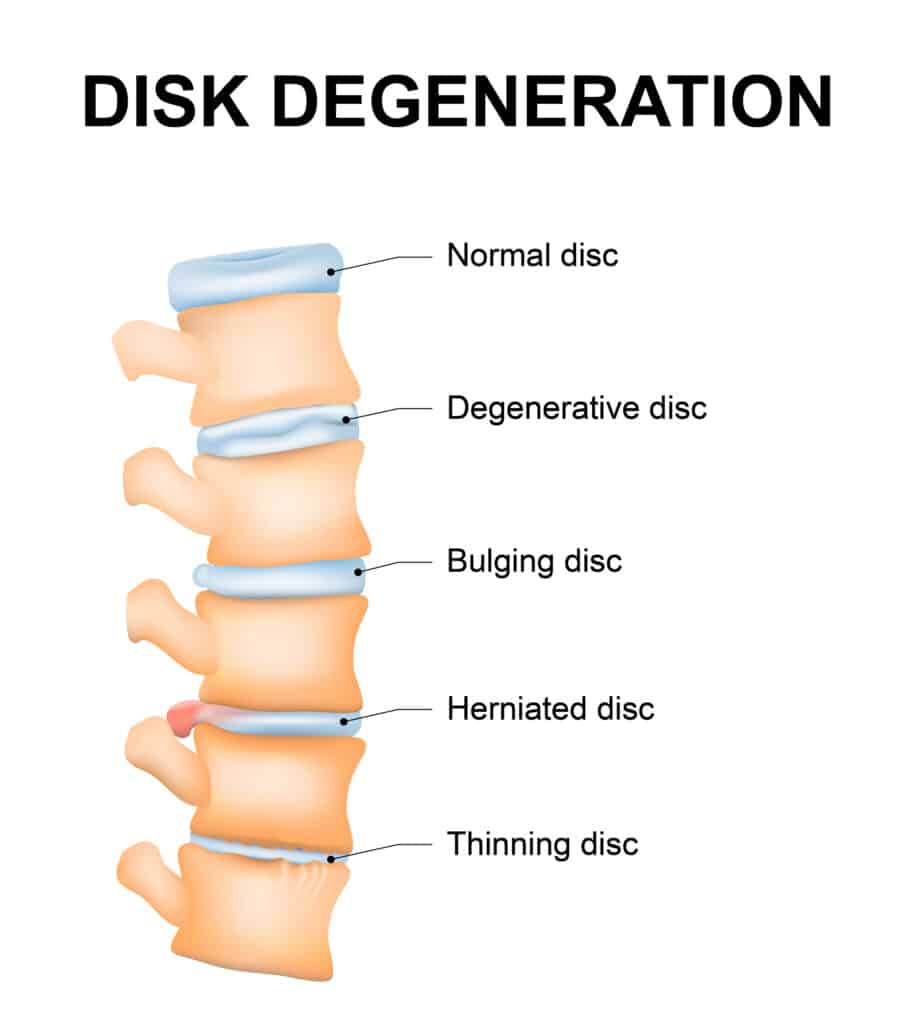
Degenerative Disc Disease Causes
Each spinal disc has a tough outer layer that contains nerves and surrounds a soft jellylike core. The spinal discs in those with degenerative disc disease typically exhibit one or more of the following changes:
- Drying out: The core of spinal discs contains a high proportion of water, and as you get older, the amount of water in them naturally lessens, making them thinner and less shock-absorbant.
- Tearing or cracking: Wear and tear or injury can cause tears or cracks in spinal discs, which can be painful, even if they’re minor.
Things to Avoid with Degenerative Disc Disease
Regular daily activities, sports, and injuries can cause degenerative disc disease. While even active and otherwise healthy individuals can be affected by the condition, certain contributing factors make some people more likely to develop degenerative disc disease, including:
- People who’ve suffered acute spinal injuries, such as sports injuries or those from a fall or impact
- People who are overweight or obese
- Women
- Smokers
- People who have physical jobs that require them to stand and exert extraneous effort for long periods
To help prevent degenerative disc disease, doctors advise that you maintain a healthy weight, don’t smoke, and exercise regularly to maintain strength and flexibility.
Symptoms
The most common symptom of degenerative disk disease is mild, moderate, or severe pain and stiffness in the neck and back. The pain typically:
- Presents intermittently, lasting for weeks or months at a time before stopping temporarily and then starting again
- Causes numbness or tingling in your arms or legs
- Radiates through your lower back and into your buttocks and legs as well as into your arms and hands
- Is exacerbated by sitting, bending over, lifting something heavy, or twisting
- Gets worse over time
- Makes you want to change positions frequently or lie down to relieve the pain
- Feels better when you’re walking or running rather than sitting or standing for long periods
What is degenerative disc disease?
To diagnose degenerative disc disease, your orthopedic spine specialist typically starts by asking about your symptoms, including:
- When did the pain first start?
- Where is the pain?
- Are there any activities or movements that bring about or increase the pain?
- Does anything work to decrease the pain?
- Did you have an accident or injury that led to the pain?
- Do you have symptoms such as tingling, numbness, or radiating pain? What about back spasms?
- Is the pain impacting your daily routine or favorite activities?
Your specialist will also perform a physical exam to evaluate your nerve function and muscular strength. The vast network of nerves in and around the spine increases the chances of pain caused by drying out or tearing and cracking, and those suffering from degenerative disc disease may show decreased nerve function due to damaged or compressed nerves. They may also exhibit muscular weakness from nerve damage or disc degeneration. Your orthopedic specialist will likely take an X-ray, CT scan, or MRI to see the condition and alignment of your spinal discs.
Degenerative disc disease is a painful condition on its own, but it can also cause other problems, including:
- Osteoarthritis
- Herniated disc: Also referred to as a slipped, ruptured, or bulged disc
- Spinal stenosis: When the spaces around your spine become more narrow
- Adult scoliosis: When the spine becomes curved
- Spondylolisthesis: When vertebrae slip in and out of place
- Spondylolysis: When you get a small crack between two vertebrae
It’s important to get care from a pain management and spine care specialist to help prevent additional issues.
Treatments
Spinal discs have a very low blood supply, so they cannot repair themselves. However, many people with degenerative disc disease successfully use at-home nonsurgical methods to manage their symptoms. Work with your pain management and spinal care specialist to find a symptom-management plan that addresses your goals and lifestyle.
Common treatments include:
- Exercise, including low-impact activities like swimming and walking, to help strengthen your back and relieve pain
- Alternating ice and heat packs about every 15 minutes several times a day to combat pain and inflammation
- Stretching, as gentle movements can alleviate tension
- Pain medications like nonsteroidal anti-inflammatories (aspirin, ibuprofen, and naproxen), muscle relaxers, or steroids
- Physical therapy to strengthen and stretch the muscles of the back and those around the spine
- Steroid injections around your nerves and discs to reduce pain and inflammation
- Radiofrequency neurotomy, a procedure that uses electric currents to prevent nerves from sending pain signals to your brain
Degenerative Disc Disease Surgery
Most people with degenerative disc disease do not need surgery, but in severe cases where nonsurgical treatments aren’t helping and pain continues to impact one’s life, surgery can be a good option. Stay active, healthy, and strong after surgery to prevent further issues.
If you have neck or back pain and would like to speak to a pain management and spine care specialist, please contact us or comment below.
Leave a Reply